Holistic Pregnancy & Childbirth

What about pain?
Pain is your body's way of telling you to take action. Consider the pain you feel when you burn yourself. The pain tells you to take your hand away from the flame! Similarly, when you sustain an injury, pain might influence you to apply ice or to get an X-ray.
Childbirth pain gives you a message: the time of birth is near. It encourages you to take action: to choose a safe place to give birth, gather your support people, and bring your baby into the world.
Childbirth pain is not like other pain
 Yet childbirth pain is very different from most other types of pain.
Yet childbirth pain is very different from most other types of pain.
- It is NOT is a signal that something is wrong. Childbirth pain helps you determine what is happening within your body, what part of labor you are in, and what actions you might take.
- It is not constant, but comes and goes as the contractions do, giving you a chance to rest and regroup.
- It is pain with a positive purpose. Childbirth pain leads to the birth of your baby, which is greatly different from the pain of injury, infection, or chronic illness.
Recognizing the powerful effect that language can play on our perception, some childbirth experts suggest renaming childbirth pain to provide a positive association related to the work being done by the body, rather than the negative association that accompanies the word pain. One noted midwife, Ina Mae Gaskins, uses the term "rushes," and in HypnoBirthing® classes, people are encouraged to talk about "surges" instead of contraction pain.

Learning to cope with pain is not a new concept for most people. Everyone has experienced pain, and most of us already have identified measures that help. Here are some ideas that may help with childbirth.
Consider techniques you have used before to alleviate pain, such as cold compresses and rest for a headache or deep breathing or distraction for an injury.
If you have already experienced labor, think about which pain management techniques were most successful to help you in preparing for childbirth again.
If you felt somewhat unsuccessful in coping with childbirth pain before, you might be scared or nervous when you think about doing it again. Take some time to acknowledge this and recognize that these are normal feelings.
For many of us, this may be culturally based. In some cultures, pregnant people are expected to be stoic about childbirth pain and may exhibit few signs of pain as they experience contractions. In other cultures, loud expressions of pain are expected. All of these responses are normal, yet some produce a greater reaction from those around you. After all, who doesn't want to help someone who is crying or moaning?
As you prepare for birth, help prepare your support people as well, by talking or role-playing with them about how you might express pain and how they might best respond to this.
Some childbirth preparation materials talk about relieving discomfort, which might lead you to believe that it will go away with proper techniques. However, most birthing people report that childbirth is hard work and painful and holistic pain management and comfort measures can seldom eliminate pain.
What they can do is give you tools to minimize the amount of pain you have, effectively cope with the pain you experience, and conserve your energy to be able to effectively do the work of childbirth.
Let yourself have your own experience with, and response to, the pain associated with childbirth.
The best preparation is to remain open and receptive to the experience, as it is impossible to predict exactly what your labor will be like.
- 1 of 6
- 2 of 6
- 3 of 6
- 4 of 6
- 5 of 6
- 6 of 6
What causes pain in childbirth?
There are three basic types of pain in childbirth. Understanding what is causing pain during the different parts of labor helps you identify the work that your body is doing. Different techniques may be necessary to cope with these different sensations.
- The first type of pain is associated with muscle contractions as the cervix is opening or dilating. During this part of childbirth, the rows of muscles in your uterus contract (shorten), pulling open the cervix. Most birthing people describe this feeling as an extremely strong menstrual cramp-like feeling. It may be felt in the lower part of the uterus, the low back, or both.
- The second type of sensation is a feeling of intense pressure as the baby gets lower and pushes on the muscles in the pelvis and on the bladder and rectum.
- The third type of pain, which occurs as the baby is being born, is a feeling of burning or stretching as the vagina and skin stretch to let the baby through.
How do fear and tension relate to pain?
 In the 1920s, Grantley Dick-Read described what has become known as the "Fear-Tension-Pain" cycle. He suggested that fear causes a birthing person to become tense, and that tension increases pain. The increased pain, in turn, increases fear, and the cycle repeats.
In the 1920s, Grantley Dick-Read described what has become known as the "Fear-Tension-Pain" cycle. He suggested that fear causes a birthing person to become tense, and that tension increases pain. The increased pain, in turn, increases fear, and the cycle repeats.
Dick-Read suggested interrupting this cycle in two ways:
- Reduce fear by educating birthing people about what is happening during childbirth
- Reduce tension by promoting relaxation, thus reducing the pain.
Most modern childbirth preparation methods have evolved from this theory.
How is pain handled in the hospital?
In United States hospitals, pain management is usually a nursing performance goal, and nurses in hospitals are expected to assess and treat pain. Hospital funding from sources such as Medicare is dependent on hospitals meeting pain management requirements.
Given this, you may be asked to "rate" your pain on a scale and offered medication if your pain is above a certain level. These measures help the hospital staff to not only treat pain, but also to meet the requirements of their review committees.
Your labor nurses might suggest medication or epidurals as measures to help cope with labor pain. Because these options are popular among laboring women, your nurses might have little experience with some holistic measures for coping with labor. On the other hand, your nurses might have a wealth of experience with alternative methods for helping people with labor.
 You can help your labor nurse and other hospital staff by:
You can help your labor nurse and other hospital staff by:
- Telling them about your plans for coping with labor soon after your arrival, and asking for their help. If you have prepared a birth plan, show it to them.
- Letting your nurses know how you express pain, especially if you find that being very vocal is helpful to you.
- Letting your nurses know what has worked for you so far in your labor and what your plans are for pain management.
- Asking for other suggestions they might have.
Ask for help in maximizing your freedom of movement
You can also ask your nurses for their help in maximizing your freedom of movement and your ability to choose comfortable positions. Some hospital practices, such as continuous fetal monitoring or IVs can limit your activity. You can ask for intermittent monitoring or a saline lock instead of a continuous IV.
If continuous monitoring becomes necessary, it does not mean you must stay in bed. You can ask to have rocking chairs and birthing balls moved close to the monitor, or to use telemetry monitoring if you wish to get into a tub or shower or walk.
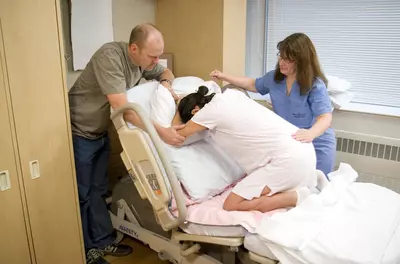
There are many things you can do to minimize the amount of pain from contractions and to cope with the pain you do feel.
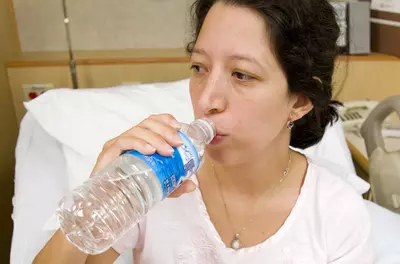
Your uterus is a collection of muscles, and like all muscles, works best with the least amount of pain when well hydrated and receiving plenty of oxygen.
You can promote blood and oxygen flow to the uterus by drinking plenty of liquids and staying off your back. (Lying on your back can reduce blood flow to the uterus by almost 30%!)

Another way to reduce the amount of pain you feel with contractions is to keep your abdominal muscles relaxed. Many childbirth preparation methods teach relaxation techniques to help during labor.
Ways to promote muscle relaxation and minimize the amount of pain you experience include progressive relaxation techniques, self-hypnosis, patterned breathing, visualization, and massage. Several weeks of practice will help these techniques become ingrained habits and easier to use during times of stress or pain.
Apply warm or cold compresses to either your back or your low abdomen to help alleviate pain.
Taking a shower or sitting in a tub to reduce pain and promote relaxation. You can sit on a stool in the shower if you are tired, and direct the flow of water at either your back or your abdomen, whichever feels best.
If using a tub, the deeper the water, the better, as you can immerse your abdomen. If your tub is shallow, try putting a towel over your abdomen and have your partner slowly pour water over the towel during contractions. Prepare in advance: find a stool that fits in your shower or tub and doesn't slip, and also try the water pouring exercise ahead of time.

During your labor, you might find that upright positions such as standing, walking, or sitting in a rocking chair or on a birthing ball (a physical therapy ball) might help you cope with contractions. Swaying or moving your hips could help, while also encouraging the baby to choose the best path through the bones of your pelvis. In general, you should follow your body's messages and choose positions that feel the best.

If you experience back pain or if your midwife, doctor or labor nurse tells you that they think the baby is in a posterior position, use this pain as a message, and try some forward leaning positions that might encourage your baby to turn. You may try lying on your side, tipped far over almost onto your stomach. Or try spending time resting on your knees and forearms, or standing and bending forward at the waist. These positions also let your partner apply firm counter-pressure to your back or hips, which may greatly help alleviate the back pain.
You can combine therapies, using forward leaning positions in the shower or tub. Or apply ice packs or warm packs to your back while leaning forward.
Your midwife or doctor could also help alleviate back pain by the use of sterile water papules, which are small injections of water just beneath the skin in your low back.
- 1 of 8
- 2 of 8
- 3 of 8
- 4 of 8
- 5 of 8
- 6 of 8
- 7 of 8
- 8 of 8
Complementary therapies to reduce labor pain
- Acupressure is another method of pain reduction some pregnant people have used very effectively during labor. A variety of pressure points may be used, and if you are interested in these techniques, you should do some advanced planning. While you or your partner may do them during labor, you might want to visit an acupressure practitioner with your partner before labor begins to make sure you understand the technique.
An excellent resource for using acupressure in labor can be found in the web publication Natural Pain Relief Techniques for Childbirth Using Acupressure, by acupuncturist Debra Bett.
- Reiki, Healing Touch, or Reflexology may be helpful during labor. You may include a practitioner of one of these methods on your birth team, or, if you have planned in advance, you may learn techniques such as Reiki yourself.
- Add a doula to your support team. A doula is a person who provides continuous support to a person in labor. They may be certified through a doula training organization and has studied a variety of techniques for coping with labor. They remains with you throughout labor, and can help you and your partner use the right technique at the right time during labor.
The use of a doula has been consistently shown to be associated with shorter labors, less use of pain medication, and fewer cesarean sections. The topic How Can I Arrange the Best Birth Support has additional information about how to find a doula.
What about pain during the last phases of childbirth?
The last stages of labor and childbirth present new experiences.
As the baby moves down in the pelvis
As your labor progresses, and your baby moves further down in the pelvis, your feelings of pressure may increase. Eventually, this feeling of pressure will change, and you may begin to feel a need to push or bear down. For some people, this feeling is subtle, for others, it is overwhelming. Again this feeling is a signal or message, telling you that it may be time to begin pushing during your contractions, to help bring your baby down further. Some people feel this phase of labor is a relief from the pain of labor contractions, as they can start responding to the contractions by bearing down, helping with the downward movement of the baby.
Generally, you may follow your body's messages and push as you feel comfortable. You may do this in a variety of positions; view examples of effective birthing positions. Your midwife, doctor, or labor nurse may help give you guidance to push effectively.
During birth
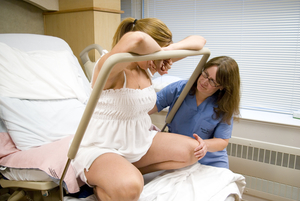 As your baby is being born, you may feel intense burning as the baby comes out. While this is normal, and signals that your vagina and skin are stretching to make room for the baby, many birthing people feel that they are tearing. Using warm wet compresses on your perineum (the skin between your vagina and anus) as you push may help guide you in knowing where to push and can alleviate some of the pain with crowning.
As your baby is being born, you may feel intense burning as the baby comes out. While this is normal, and signals that your vagina and skin are stretching to make room for the baby, many birthing people feel that they are tearing. Using warm wet compresses on your perineum (the skin between your vagina and anus) as you push may help guide you in knowing where to push and can alleviate some of the pain with crowning.
Your midwife or doctor can provide verbal guidance as you to push gently as the head is being born (called crowning) to help minimize any tears. The good news about this burning is that it is short lived, lasting only a few contractions at most.
Especially for first time mothers, doing perineal massage (massage of the skin around the back of the vagina) during pregnancy can help prevent tears, and give you some feeling of what this stretching sensation feels like. You can read about performing perineal massage and see some pictures at the University of Michigan's School of Nursing website. Either you or your partner may perform the massage.
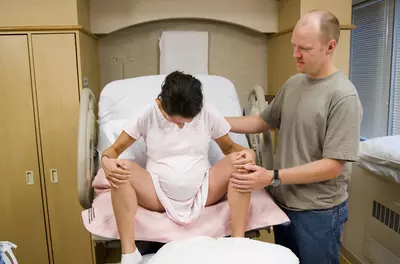
Birthing positions
There are several birthing position options to consider. View these photos and read their descriptions to help prepare for childbirth.
Sample birth plans
Read these sample birth plans to help make your own.
Sample Birth Plans
Sample Birth Plan 1
To my midwife and labor nurses:
Welcome to my birth plan. I am Ginny Snell. My partner is Charles Peterson, and we will also be accompanied by our birth assistant, Cindy Smith.
I am a first time mother, so I am very curious to experience labor. I also tend to be a very cautious person. Charles is more adventuresome. We have done much preparation and hope to allow labor to progress at its own pace. We welcome your suggestions at any point. We plan to be flexible and hope that you will too.
First Stage:
- I would like to spend my early labor at home. If you think that I have arrived at the hospital in early labor, I would like to return home.
- I would like to eat and drink throughout labor if I feel like it. Please remind me to drink if I forget.
- My primary plan to cope with pain is to use movement and water. To help me with freedom of movement, I would like the baby monitored intermittently. Charles and Cindy may also help with relaxation techniques.
- I would like to use natural techniques to stimulate labor if necessary, such as nipple stimulation, before considering medications.
Second Stage:
- I would like to follow my own urges to push in whatever position I find comfortable.
- Please make suggestions if you think I could do something more effectively.
- After the baby is born, Charles would like to help move the baby onto my abdomen and cut the cord.
Our wishes for our baby:
- I plan to breastfeed the baby without bottles. I'd like to wait several weeks before I try a pacifier.
- Charles would like to give the baby the first bath.
- If our baby is a boy, we would like him to be circumcised, but only after we have successfully breastfed several times. Charles and I would like to be present and would like the baby to receive anesthesia for the surgery.
Sincerely,
Ginny and Charles
Sample Birth Plan 2
Dear Dr. Cox, my anesthesiologist, and my birth nurses:
I know you might be surprised to read a birth plan because, as you know, we are planning a repeat cesarean section. However, I do have some specific requests regarding my surgery and hospital stay that I hope you will consider.
I will be accompanied by my parents, Sue and Tim Lee. If possible, I would like to have both of them with me in the delivery room. In my family, it is traditional for the oldest male to be involved in making medical decisions, and I am comfortable with this. If any treatment decisions need to be made, please include my father in the discussion. We are adapting to new traditions, however, and if my father and I cannot agree on a plan, I will make the final decision. My father knows this, but he will be uncomfortable. Please be understanding of him.
I would like my baby to remain in the operating room and recovery area with me after she is born. I realize that this may require having an additional nurse assigned and that this might not be possible on a very busy day. But if possible, I hope that this request can be accommodated.
Anesthesia requests:
- I would like to receive a spinal or epidural anesthesia for my birth, and would like to avoid receiving any medications after the birth that would make me drowsy or unable to interact with my baby.
- I was very nauseated after my first cesarean birth, and would like you to plan for this and premedicate.
Post-birth requests:
- If we could dim the lights in the recovery area to encourage my new baby to open her eyes I would appreciate this.
- My mother will be remaining with me to help me care for the baby until I am able to be up and out of bed.
- I would like to breastfeed exclusively.
- Please remind me to take pain medication. I tried to go without last time, but I think it will be more helpful, and I will be more comfortable during my recovery if I take it.
Sincerely,
Karen Lee

Questions for your midwife or doctor
Review these questions with your midwife or doctor
Questions for your Midwife or Doctor
As you talk with a potential midwife or doctor, here are some things to consider asking.
Credentials and Privileges
- Is the provider board-certified, and if so by what organization?
- Where does the provider attend births (what hospitals or other facilities)?
- If the provider is a home-birth provider, and what systems are in place for consultation or transfer if that becomes necessary?
Childbirth Practices
- Does the provider have preferences regarding eating and drinking in labor?
- How does the provider monitor your progress during labor?
- How does the provider monitor your baby's well-being during labor?
- Does the provider offer any complementary therapies? If so, what are they, and are there any limitations on their use?
- Does the provider support waterbirth? If so, are there limitations on who may give birth in the water?
- Does the provider have any restrictions on positions that you can give birth in?
- Does the provider typically take the foot of the bed off for birth, or leave it in place?
- What medical methods of pain relief does this provider typically use?
- If your provider practices in a group, might you see a different provider at birth? If so, how are differences in philosophy between group members dealt with?
Provider Statistics
- How much time does the provider schedule for each prenatal appointment?
- What is the provider's induction rate? Why are women typically induced?
- What is the provider's epidural rate?
- What is the provider's cesarean section rate?
- What percentage of the provider's patients has an episiotomy?
- Does the provider practice within a group, and, if so, how large is the practice?
- If the provider practices within a group, what are the rates of the above interventions for the group?
- What percentage of the provider's patients give birth without using any medication or epidural for pain?
Hopefully, the answers to the above questions will let you ask these questions of yourself:
- Did the provider welcome your questions?
- What does this provider's attitude toward holistic childbirth seem to be?
- Did the provider appear to trust the birth process?
- Did you feel patronized or put down by any of the answers?
What if I can't cope without pain meds?
Not every technique will work for every birthing person, and each labor is unique. Adopting a holistic approach to childbirth, by the very definition of the word "whole," may also mean considering the use of pain medication, or epidural or intrathecal (spinal) anesthesia.
Even if you don't think you will use them, ask your midwife or doctor what pain relief methods they commonly use, so that you can read about their benefits and risks before labor begins. Be sure to review the topics Why Should I Consider Holistic Childbirth and What Factors Influence the Natural Progression of Childbirth, as they contain information about the potential risks and benefits of pain medications and epidural anesthesia. If you begin to think about using medication during labor, keep the following guidelines in mind.
- Try not to make a decision at the peak of a contraction, but use the time between contractions to discuss what you've tried so far and what you might like to consider. Sometimes, more support can make a difference.
- Ask your nurse, midwife, or doctor not to offer pain medication while you are having a contraction.
- Consider how far along you are in labor: perhaps ask to have your cervix checked. If you know that you may only have a little time to go, this might influence your decision.
- Recognize that the use of medication is simply a technique at the end of a continuum, and not evidence of personal failure or failure of the use of other techniques. Remember that by using a variety of pain reduction techniques prior to medication, you reduce the amount of medication you take and thus the risks involved.
References
Albers LL. (2007). The evidence for physiologic management of the active phase of the first stage of labor. Journal of Midwifery & Women's Health. 52(3), 207-215.
Caton, D., Corry, M.P., Frigoletto, F.D., Hopkins, D.P., Lieberman, E., Mayberry, L., Rooks, J.P., Rosenfield, A., Sakala, C., Simkin, P., Young, D. (2002). The nature and management of labor pain. American Journal of Obstetrics & Gynecology, 186(5), S1-S15.
Additional Readings
http://www.childbirthconnection.org/
Childbirth Preparation Books:
Active Birth: The New Approach to Giving Birth Naturally, Revised ed. 1992. Janet Balaskas. Harvard Common Press.
Birthing from Within. 1998. Pam England, CNM. Partera Press.
Ina May's Guide to Childbirth. 2003. Ina May Gaskin. Bantam.
Natural Childbirth the Bradley Way, Revised ed. 1996. Susan McCutcheon-Rosegg. Plume.
Pregnancy, Childbirth and the Newborn: The Complete Guide. 2001. Penny Simkin. Meadowbrook.
The Thinking Woman's Guide to a Better Birth. 1999. Henci Goer. Perigee Trade.
Especially for your partner:
The Birth Partner, 2nd Ed. 2001. Penny Simkin. Harvard Common Press.